Antibiotics
Posted: Tue Jan 30, 2007 2:33 pm
Originally posted by 'kr105' at PlanforPandemic

Antibiotics
* Link Unavailable. This site is no longer active and available to view on line. But the info was good and we wanted to keep sharing it!
 (kr105)
(kr105)
Antibiotics have a "spectrum" of bacteria that they kill. THis is usually due to their mechanism of action. If you remember microbiology, you'll remember that bacteria can be gram positive or gram negative. So the drugs are broken down into broad categories, depending on their base drug and what they can kill. I've outlined them below with representative drugs from each category.
1) Penicillian Family: 4 generations of medications
1st gen (peniciliin): gram positive strep. and oral microbes
2nd gen (dicloxacillin): gram positive strep and staph aureus
3rd gen (amoxil, augmentin): gram positive strep, some gram negative bacteria
4th gen (ticar): pseudomonas
2) Cephalosporins: 4 generations of medications
1st gen (Keflex): kills gram positive bac. and limited gram negative
2nd gen (cefzil, ceclor): kills gram positive (but less effective on staph. aureus), better gram neg. coverage and some aneorbic coverage
3rd gen (omnicef, rocephin): limited gram positive coverage, better gram negative coverage and limited pseudomonas
4th gen (cefepime): Pseudomonas coverage, good gram negative coverage but limited gram positive coverage.
3) Macrolides: This is a group with specific coverages. Some of their drugs include:
-- Azithromycin (z-pack) covers gram positive (staph aureus - non MRSA) very limited gram negative coverage(will not work against E. Coli). First line therapy for community acquired pneumonia.
-- Clarithromycin (Biaxin) similar in coverage to Azithromycin but with even less gram negative coverage.
-- Erythromycin: similar to azith and clarith above.
4) Quinolones (THe BIG guns) CDC has requested that providers not use these as first line therapy because of raising resistence rates. 4 generations of medications:
1st gen (Nalidixic acid): gram negative (not pseudomonas)
2nd gen (Cipro, Floxin etc.): gram negative with pseudomonas), some atypicals
3rd gen (Levaquin): gram negative with pseudomonas, limited gram positive including staph aureus & pneumococcus, atypicals
4th gen (tecquin, avelox): gram negative, gram positive, decreased pseudomonas, increased pneumococcus
There are also sulfa drugs, tetracyclines and a bunch of stand alones (like Macrobid, flagyl and vancomycin)
The two pocket references that I use in clinic the most are Sanford's guide to antimicrobial therapy (tells you which drugs works against which bug) and the pocket pharmacopoeia which gives you dosing.
What folks go to medical school to learn, is what bugs cause what illnesses. It takes years to learn that. Once you know what causes what illnesses, then it's over to the pocket references to write a prescription.
THE MOST IMPORTANT ASPECT OF GOING ON ANTIBIOTICS IS TO TAKE THE ENTIRE PRESCRIPTION AS DIRECTED. We have such a high rate of resistence because folks felt better, (& thought they knew better than the provider) and stopped the medication early.
When you are very ill, you have millions of bacteria in your body. When you feel better and stop taking the medication (say around day 7) you only have hundreds of bacteria left. All it takes is one to survive, that is now resistent to that class of antibiotic. It will multiply, and we have a resistant infection. PLEASE TAKE ALL MEDICATION AS DIRECTED
 (2cats)
(2cats)
kr,
Would you give us some suggestions about the best ways to store antibiotics at home?
 kr,
kr,
Most medications will last longer if you put them in the fridge. The cold temp will slow down the chemical reactions that degrade the medication.
Most pharmacies automatically put a 6 month shelf life on the label. This is not nec. accurate. I pulled the foil packet out of a z-pack folder and the actual expiration date was a year later than the pharmacist listed on the label. If in doubt, email the manufacturer and ask them when it will expire (Caveat: Amoxil liquid is only good for a few weeks once it is in liquid form.)

Antibiotics
* Link Unavailable. This site is no longer active and available to view on line. But the info was good and we wanted to keep sharing it!
Antibiotics have a "spectrum" of bacteria that they kill. THis is usually due to their mechanism of action. If you remember microbiology, you'll remember that bacteria can be gram positive or gram negative. So the drugs are broken down into broad categories, depending on their base drug and what they can kill. I've outlined them below with representative drugs from each category.
1) Penicillian Family: 4 generations of medications
1st gen (peniciliin): gram positive strep. and oral microbes
2nd gen (dicloxacillin): gram positive strep and staph aureus
3rd gen (amoxil, augmentin): gram positive strep, some gram negative bacteria
4th gen (ticar): pseudomonas
2) Cephalosporins: 4 generations of medications
1st gen (Keflex): kills gram positive bac. and limited gram negative
2nd gen (cefzil, ceclor): kills gram positive (but less effective on staph. aureus), better gram neg. coverage and some aneorbic coverage
3rd gen (omnicef, rocephin): limited gram positive coverage, better gram negative coverage and limited pseudomonas
4th gen (cefepime): Pseudomonas coverage, good gram negative coverage but limited gram positive coverage.
3) Macrolides: This is a group with specific coverages. Some of their drugs include:
-- Azithromycin (z-pack) covers gram positive (staph aureus - non MRSA) very limited gram negative coverage(will not work against E. Coli). First line therapy for community acquired pneumonia.
-- Clarithromycin (Biaxin) similar in coverage to Azithromycin but with even less gram negative coverage.
-- Erythromycin: similar to azith and clarith above.
4) Quinolones (THe BIG guns) CDC has requested that providers not use these as first line therapy because of raising resistence rates. 4 generations of medications:
1st gen (Nalidixic acid): gram negative (not pseudomonas)
2nd gen (Cipro, Floxin etc.): gram negative with pseudomonas), some atypicals
3rd gen (Levaquin): gram negative with pseudomonas, limited gram positive including staph aureus & pneumococcus, atypicals
4th gen (tecquin, avelox): gram negative, gram positive, decreased pseudomonas, increased pneumococcus
There are also sulfa drugs, tetracyclines and a bunch of stand alones (like Macrobid, flagyl and vancomycin)
The two pocket references that I use in clinic the most are Sanford's guide to antimicrobial therapy (tells you which drugs works against which bug) and the pocket pharmacopoeia which gives you dosing.
What folks go to medical school to learn, is what bugs cause what illnesses. It takes years to learn that. Once you know what causes what illnesses, then it's over to the pocket references to write a prescription.
THE MOST IMPORTANT ASPECT OF GOING ON ANTIBIOTICS IS TO TAKE THE ENTIRE PRESCRIPTION AS DIRECTED. We have such a high rate of resistence because folks felt better, (& thought they knew better than the provider) and stopped the medication early.
When you are very ill, you have millions of bacteria in your body. When you feel better and stop taking the medication (say around day 7) you only have hundreds of bacteria left. All it takes is one to survive, that is now resistent to that class of antibiotic. It will multiply, and we have a resistant infection. PLEASE TAKE ALL MEDICATION AS DIRECTED
kr,
Would you give us some suggestions about the best ways to store antibiotics at home?
Most medications will last longer if you put them in the fridge. The cold temp will slow down the chemical reactions that degrade the medication.
Most pharmacies automatically put a 6 month shelf life on the label. This is not nec. accurate. I pulled the foil packet out of a z-pack folder and the actual expiration date was a year later than the pharmacist listed on the label. If in doubt, email the manufacturer and ask them when it will expire (Caveat: Amoxil liquid is only good for a few weeks once it is in liquid form.)

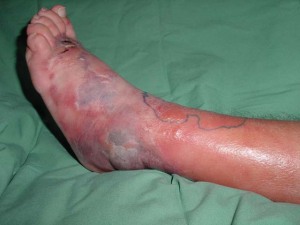 “The first rule of antibiotics is try not to use them, and the second rule is try not to use too many of them.” - Paul Marino The ICU Book 2007
“The first rule of antibiotics is try not to use them, and the second rule is try not to use too many of them.” - Paul Marino The ICU Book 2007


 One of the most common questions that I am asked from prospective survival medics is “What antibiotics should I stockpile and how do I use them?” There isn’t a 60 second answer to this. Actually, there isn’t a 60 MINUTE answer to this, but anyone that is interested in preserving the health of their loved ones in a collapse will have to learn what antibiotics will work in a particular situation.
One of the most common questions that I am asked from prospective survival medics is “What antibiotics should I stockpile and how do I use them?” There isn’t a 60 second answer to this. Actually, there isn’t a 60 MINUTE answer to this, but anyone that is interested in preserving the health of their loved ones in a collapse will have to learn what antibiotics will work in a particular situation. One of the most common questions that I am asked from prospective survival medics is “What antibiotics should I stockpile and how do I use them?” There isn’t a short answer to this. Actually, there isn’t even a long answer to this, but anyone that is interested in preserving the health of their loved ones in a collapse will have to learn what antibiotics will work in a particular situation. This is part 2 of a series on the most important antibiotics to have in a collapse situation and how to use them.
One of the most common questions that I am asked from prospective survival medics is “What antibiotics should I stockpile and how do I use them?” There isn’t a short answer to this. Actually, there isn’t even a long answer to this, but anyone that is interested in preserving the health of their loved ones in a collapse will have to learn what antibiotics will work in a particular situation. This is part 2 of a series on the most important antibiotics to have in a collapse situation and how to use them.






